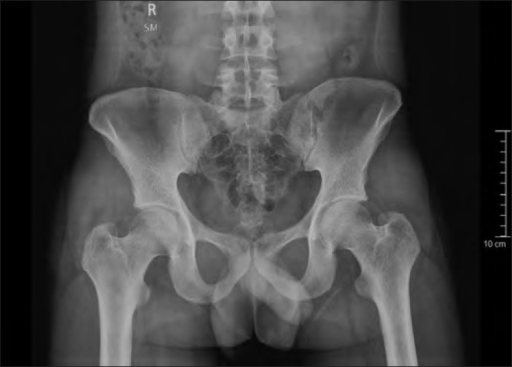
This article aims at a missing, more complete assessment of benefits and risks of gonad shielding, from its beginning until now. The Dutch guidelines provide steps in these directions, as does the work by Frantzen et al. This debate should ideally be decided by a quantitative analysis based on proper knowledge of radiation risks, reduction in hereditary risk by gonad shielding and the increase in risk caused by negative side-effects of shielding. Other authors dismiss gonad shielding partly or express their doubts about existing benefits. The ICRP (2013) and IAEA (2018) endorse this practice, whereas others, such as the Dutch guidelines, Marsh and Silosky and the AAPM, no longer recommend it. The benefit of gonad shielding in anteroposterior (AP) pelvic radiography is currently under debate. Discontinuation of gonad shielding seems therefore justifiable. For men, there might be a marginal benefit, but potential negative side-effects may well dominate. Today, using a modern and optimised X-ray system, gonad shielding can be safely discontinued for women. Optimisation likewise contributed, but unfortunately, its potential was never adequately exploited. ConclusionsĪssessment of pelvic doses revealed a large reduction in radiation risks facilitated by technological developments. Imaging-chain improvements over time were considerable: in 2018, the absorbed dose was 0.5% of its 1905 value for the testes and 2% for the ovaries, our optimised effective dose a factor five lower than the value corresponding to the current EU diagnostic reference level, and the reduction in detriment-adjusted risk by shielding less than 1 × 10 −6 for women and 5 × 10 −6 for men. In the 1950s, concerns about hereditary risks intensified and gonad shielding was recommended again, becoming routine worldwide. In the 1900s, gonad shielding was first applied to prevent male sterility, but was discontinued when instrumental developments led to reduced radiation doses. Based on own pre-1927 dose reconstructions, reported doses after 1927, a 2015-report from the European Union and recent own measurements, the effects of technological evolution and optimisation on radiation dose and hereditary risk were assessed.
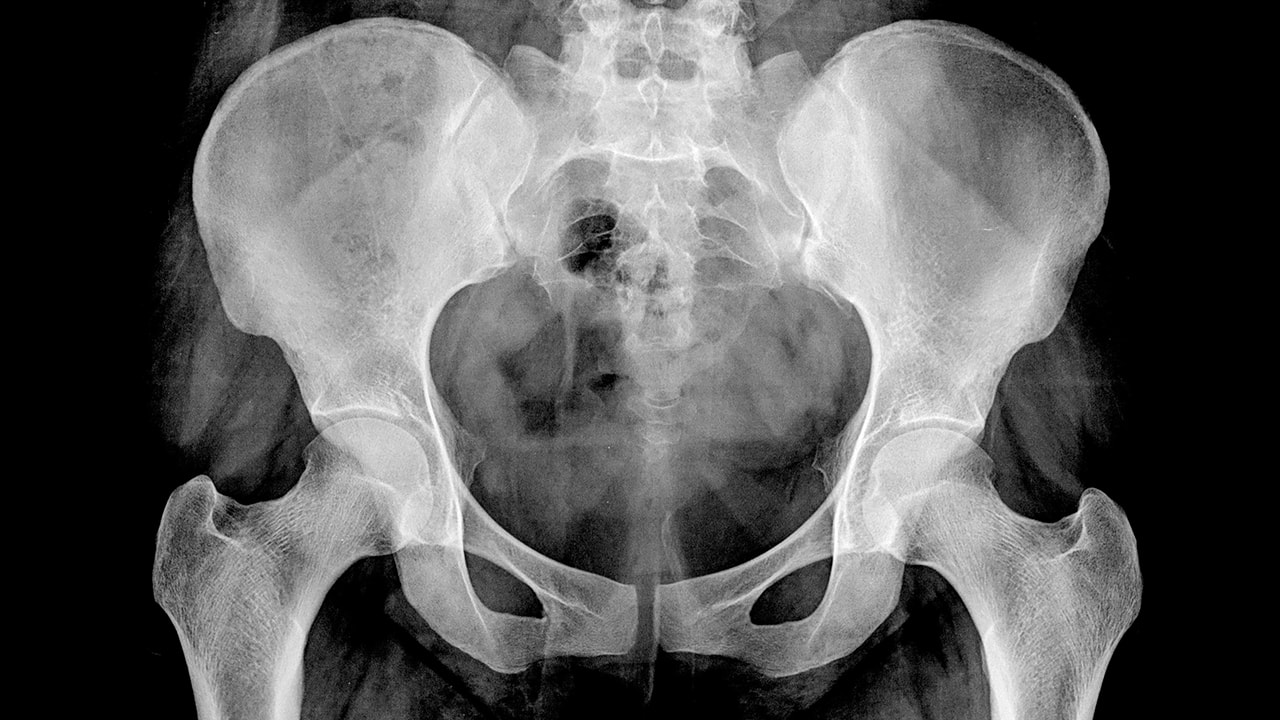
The literature was searched for developments in shielding and insights into the effects of ionising radiation on gonads. The AP of the whole pelvis (not shown on the X-rays on this page) should be fully assessed because pelvic fractures can mimic the clinical features of a hip fracture.As gonad shielding is currently under debate, this study evaluates the practice, from its introduction in about 1905 until today. Standard viewsĪP (Anterior-Posterior) pelvis and Lateral hip. Particular care is needed in assessing the X-ray when physical examination is limited, for example if a patient is acutely confused. Repeat X-rays, CT or MRI may be required if pain persists. In this case the X-ray may not show an obvious fracture. It is important to be aware that the common clinical signs of a shortened and externally rotated leg may be absent if the fracture is not displaced. Many hip fractures are clinically and radiologically obvious. Remember to assess the surrounding pelvic bonesįractures of the proximal femur or 'hip' are a common clinical occurrence in elderly, osteoporotic patients.Particular caution is required in the case of acutely confused patients.Not all hip fractures are visible on the initial X-ray and follow-up imaging may be required if concern remains.
